
These exlusions included reoperation due to local pain (n=19), revision closed reduction percutaneous pinning (CRPP) (n=2) and subsequent adjacent fracture (n=6) 6. The one study found that failed to demonstrate any statistical significance between posterior tilt and fracture failure did not include 27 of the 45 reoperations in their analysis 6. The evidence against posterior tilt predicting fixation failure in Garden I and II fractures is scarce. This agreement rate is improved with availability of both plain radiograph and CT imaging9. High interobserver agreement for measuring posterior tilt on plain radiographs and CT have been shown 9. Gender has also proved to be a non- statistically significant indicator of failure. 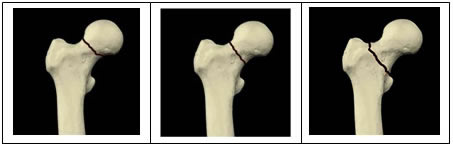
Increasing age has also correlated to fixation failure, but in many studies, this was not statistically significant. Another study showed statistical significance of failure with any degree of posterior tilt 2. This study demonstrated increased failure with increasing posterior tilt but only found statistical significance at posterior tilt above 20 degrees 3. One study in particular divided populations into 3 groups of posterior tilt angle, 0-9, 10-19 and greater than 20 degrees 3. Many studies have found posterior tilt angles greater than 20 degrees to correlate with a higher rate of complication or failure 3,5,7,8. Results: Posterior tilt angle has shown to be a statistically significant predictor of fracture failure in Garden I and II fracture pattern s1-5,7. Studies included examine the posterior tilt angle in Garden I and II fracture patterns with a primary goal to extrapolate data and report significant conclusions as compared to other predictors of outcomes in the Garden I and II fracture population. Through metanalysis, with searches directed through the PubMed database, this paper examines prospective and retrospective systematic reviews, cohort studies and case control studies and reports the data found. Methods: The posterior tilt angle is measured as an angle between the mid-column line and the radius-column line on a lateral radiograph 5. Failure of internal fixation in Garden I and II fractures requires subsequent operative interventions A primary treatment plan of hip arthroplasty may be beneficial in patients with nondisplaced femoral neck fractures with increasing posterior tilt to avoid postoperative complications and subsequent surgery 7. These recent findings discussed in this metanalysis hold significance to orthopedic surgeons treating hip fractures, as posterior tilt is not currently factored into the Garden classification system which classically guides treatment for femoral neck fractures. High Interobserver agreement for measuring the posterior tilt angle has been demonstrated amongst orthopedic surgeons 4. This angle is clearly illustrated in figure 1 and can be measured on radiograph as well as on CT scan as seen in figure 2. The posterior tilt angle is measured on the femoral neck as an angle between the mid-column line and the radius-column line on a lateral radiograph 5. A new measurement, the posterior tilt angle has been recently discussed as a specific measurement to guide treatment specifically in nondisplaced femoral neck fractures 1-5,7. Age, ASA score and gender have previously been discussed as predictors of outcomes, but data is not consistent. There is a paucity of evidence to support objective factors that can be attributed to this rate of failure. Complications however are not uncommon and failure rates of internal fixation in this fracture population can approach 20% 1. Introduction: Internal fixation with cannulated screws has long been the standard of care for Garden I and II femoral neck fractures 1. Kiran C Patel College of Osteopathic MedicineĢPhiladelphia College of Osteopathic Medicine – Department of Orthopedics By Nicholas Lampasona OMS-III 1, Drew Papadelis DO, PGY-2 2ġNova Southeastern University Dr.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
